Mr Sampson’s Care
 Mr. Sampson was admitted to the Phoenix VA hospital. He has been in hospital for 7 days and is about to be discharged. The plan is to try to find him temporary housing so he can continue to receive necessary care over the next weeks and months.
Mr. Sampson was admitted to the Phoenix VA hospital. He has been in hospital for 7 days and is about to be discharged. The plan is to try to find him temporary housing so he can continue to receive necessary care over the next weeks and months.
The links below provide you with information concerning the care provided to Mr.Sampson from the various professions involved in his care during his hospital stay. It also contains information on professions who may be able to play a role in his future care along with notes from his most recent dental screening.
Learn more about the Phoenix VA Hospital
Case Notes
Hospital Care Notes
Medicine/PA
Physician & Physician Assistant
Admit H&P
Name: BradleyLeonard Sampson, prefers “Butch
Age: 73M
HPI: This 73 yo male assessed and referred to the VA Emergency department by the Healthcare for Homeless Veterans Office with a history of Type 2 Diabetes with peripheral neuropathy, peripheral vascular disease with past hx of foot ulceration, osteomyelitis and left 4thand 5thtoe amputations. Pt reports feeling feverish for ten days with bilateral burning foot pain, x 2-3 weeks “from wearing tight shoes”. Pt reports numbness, intermittent paresthesias/burning sensation in both feet “for many years” Symptoms are similar to those he had in the past associated with toe amputations in approximately 2015. Pt reports that metformin and insulin were stolen so he has not taken these medications for the past month. Prior to that time, he took medications intermittently, did not have a refrigerator to store insulin. Pt reports polydipsia, polyuria, and polyphagia for the past six months.
PMH:
Illnesses: T2DM x 5years, History of depression, anxiety, and panic attacks x many years declined evaluation and treatment in past-not taking medications –willing to seek help. “Back injury in 1985” did not require surgery. Reports 2 falls- in the past several months-did not hit head, denies injuries from fall, no treatment sought
Injuries: Injured his back lifting cement bags in 1985
Hospitalizations/Surgeries: Left 4th and 5th toes amputated at VA hospital unsure of date possibly 2015
Medications:
- Metformin 1000 mg PO BID
- Insulin Lantus 10 Units SQ QD x 1 month
- Benadryl 25-50 mg at HS prn insomnia
- APAP 1000mg prn Q6 hrs prn back pain
Allergies: No allergies to medication, environment, or food
Prevention:
- Diet “anything I want and can get without cooking”
- Does not have a PCP, has not seen a podiatrist “for years”, no eye exam “for years”, last dental exam years ago
- Immunizations: pt cannot recall
Personal/Social History:
Occupation: retired heavy construction worker, served in armed services, Navy
Marital Status: Divorced x 2, has not been in a relationship or sexually active x10 years
Support: Homeless. Support from fellow homeless veterans, friend Joe, no children
ETOH: “couple of beers” occasionally
Tobacco: Smokes 1pack a day x 30 years
Illicit drugs: denies
Family History: Adopted, not aware of family history. No children.
Review of Systems:
Constitutional: Denies fatigue, weight loss/gain, chills, night sweats.
Eyes: Denies vision change, pain, redness.
ENT: Denies headache, hoarseness, sore throat, epistaxis, sinus symptoms, hearing loss. Tinnitus both ears X 15 years+.
Skin: Erythematous lesion on dorsal aspect of left great toe with purulent discharge and swelling x 2-3 weeks Denies rash, pruritis..
CV:Denies chest pain, PND, orthopnea, palpitations, claudication, or general LE edema
Pulm: Denies cough, SOB, wheezing, hemoptysis
Endocrine: Has polydipsia, polyphagia, polyuria. Denies heat/cold intolerance, hair/voice changes.
GI: Denies Abd pain, stool changes, N/V, diarrhea, constipation, heartburn, hematochezia, melena.
GU: Denies Dysuria, hematuria, discharge.
MSK: Hx of Intermittent low back pain-muscle spasms-none now. Denies arthralgia, arthritis, joint swelling, myalgias,.
Neuro/psych: has insomnia described as trouble getting to sleep- onset 4-5 years ago. has numbness, some paresthesia/burning sensation in both feet. Denies weakness, seizures, tremor, syncope, History of anxiety, depression, panic attacks, and memory loss for many years-overall staying the same-willing to seek help now-has anhedonia, denies depressed mood, irritability, psychomotor changes, suicidal or homicidal ideation. Has persistent and unrelenting anxiety, difficulty concentrating, and panic attacks-last attack yesterday
Heme/Lymph: Denies bleeding, bruising, clotting, transfusions, lymph node swelling
Physical Exam:
- BP: 136/74mmHg
- P: 89/min regular
- R: 18 unlabored
- T: 101.0 F
- O2Sat: 95% on RA
- BMI 36 Weight 230, height 5’7”
General: A&Ox3, cooperative, no acute distress, disheveled appearance, calm and cooperative demeanor
HEENT:
Eyes: PERRL, EOMI, Fundi without lesions, normal disc; sclera anicteric; conjunctivae pink
Ears: TMs pearly grey with normal mobility mild cerumen bilaterally,
Nose: nares patent, nasal mucosa pink, no d/c
Mouth: with pink moist mucosa, uvula midline, poor dentition with caries
Neck: supple, no bruits, thyroid symmetrical without enlargement or tenderness, no lymphadenopathy
CV: RRR without MRG.
Pulm: Lungs CTAB without adventitious sounds
Abd: Soft and NT without HSM; No scars or lesions
Extremities: Peripheral pulses: DP, PT, radial 2+ and equal bilat in upper and lower extremities. normal hair distribution on calves; no bruits, no clubbing, cyanosis full AROM all extremities . 10 gm monofilament 0/10 bilaterally. Vibratory sense impaired bilat great toes
Skin: 2.5 x 2.5 cm wound medial left great toe dorsal aspect with erythema, inflammation, induration, purulent secretion, and grossly visible bone,
GU/Rectal: Perianal external normal, Normal tone, formed brown stool neg for OB. Uncircumcised male with no lesions or d/c; Testicles symmetric, NT, no masses.
Neuro: CN II-XII grossly intact, MMSE 26/30
Labs
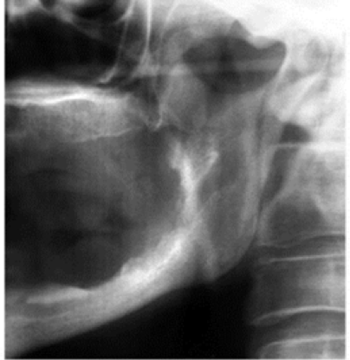
White blood count is 14,000 cell/m3, serum glucose is 280mEq/dL. HGA1c 10, ESR 110 mm/hr, comprehensive metabolic panel pending. Radiologic findings: AP radiograph of left foot shows significant soft tissue swelling over the head of the first metatarsal and base of the great toe. There is also significant bony erosion in this region with a loss of normal cortical bone, periosteal elevation, and lytic changes consistent with osteomyelitis.
Assessment:
- Left great toe ulcer due to diabetes with osteomyelitis-dorsal aspect
- T2DM uncontrolled
- Tobacco use-30 pack year history
- Personal history of mental disorders- anxiety, panic attacks, history of depression and memory loss
Plan:
- Admit to Medicine
- Diagnosis: 1) Left great toe ulcer due to diabetes with osteomyelitis-dorsal aspect 2) T2DM uncontrolled
- Condition: Fair
- Code status: Full with Fall risk precautions
- Allergies: NKDA
- VS q Shift
- Activity: OOB ad lib
- Nursing: wound care right great toe QD. Accuchecks AC and HS
- Diet: 1800 calorie ADA
- IV: 0.9% NS to KVO
- Antibiotic medications to be prescribed after renal panel results are back, plan to start antibiotics after bone biopsy/aspirations, and blood cultures are acquired.
- Fingerstick BGs AC and HS with sliding scale insulin Lispro: Goal Blood Glucose is <150. BG 150-199: 1unit bolus Insulin Regular. BG 200-249: 2 units bolus Insulin Regular. BG 250-299: 3 units bolus Insulin Regular. BG 300-349: 4 units bolus Insulin Regular. BG Over 350: 5 units bolus Insulin Regular.
- Nicotine transdermal patch 21mg daily in morning
- MOM 30 cc po prn constipation.
- APAP 650 mg po q 6hr prn mild pain or fever.
- Ambien 10 mg PO Qhs prn insomnia
- Labs: Blood cultures x 2 sites now. CBC, BMP q AM
- Consult Orthopedic surgeon for surgical drainage and debridement,
- Consult Podiatry and PT re: wound care
- Consult with psych for anxiety, panic attacks, hx of depression and memory loss
Bob Jones, PA-C
Nursing
“Nursing encompasses autonomous and collaborative care of individuals of all ages, families, groups and communities, sick or well and in all settings. Nursing includes the promotion of health, prevention of illness, and the care of ill, disabled and dying people. Advocacy, promotion of a safe environment, research, participation in shaping health policy and in patient and health systems management, and education are also key nursing roles. (ICN, 2002)
Nursing Plan of Care
Nursing Diagnoses
|
Nursing Outcomes
|
Nursing Interventions
|
Care Plan Discharge EvaluationWound healing secondary intention. -Purulent drainage 3- moderate. Foul wound odor 2- limited. -Decreased wound size 3- moderate. Surrounding skin erythema 3- moderate |
| Impaired physical mobility R/T left toe amputations and wound. Risk for falls- risk factors- history of falls, homelessness, unfamiliar setting. |
Mobility and ambulation. 1.Will have improvement in balance when ambulating. 2.Will be able to ambulate with or without assistive device to BR and back and 200 feet in hallway at moderate pace. Fall occurrence and Fall Prevention Behavior 1.Will not fall while walking. 2.Will have ability to identify and avoid obstacles. 3. Will verbalize strategies to avoid fall. |
1.Consult with PT to identify need for assistive devices and to set goals for ambulation. 2. Ambulate with pt using gait belt 200 feet BID. 3. Teach patient to call for assistance before getting out of bed. 4.Teach patient about hazards outside the hospital environment to avoid or take care: rugs, curbs, uneven sidewalks, etc. 5. Ensure call light and personal effects are within reach before leaving room and at hourly rounds. |
Fall occurrence: 5- no falls while in hospital. Fall Prevention Behavior: -Ask for assistance 3- sometimes demonstrated -Uses grab bars/ handrails- 4-5 often demonstrated. -States need to take care on uneven surfaces 4- often demonstrated. Mobility: -Balance:2- Substantially compromised -Walks moderate distance at moderate pace- 2- substantially compromised. |
| Readiness for enhanced self-care. Expresses desire to have foot heal and prevent future wounds/ issues. | Self-care status: 1.Will recognize safety needs in environment. 2. Will verbalize need to attend all out patient appointments for wound care and antibiotics. 3. Will quit or cut down smoking. Will manage diabetes to keep blood sugars < 200. Will not develop more foot wounds. 4. Will not be re-hospitalized in next year. |
1. Consult with case management about transportation resources available to patient. 2. Teach patient and ensure demonstration of blood sugar management and insulin administration. 3. Teach patient to count carbohydrates- provide table for common foods- encourage foods high in protein- discuss foods he likes that are lower in carbohydrates |
-Manages parenteral meds- 4- mildly compromised. Manages non parenteral meds- 5- not compromised. -Nutritional status: Food intake- 5- no deviation. -Fluid intake- 5- no deviation. -Knowledge Diabetes management: medication therapeutic effects- 4- substantial. -Preventive foot care practices- 2- limited knowledge. -Benefits of disease management-3- moderate knowledge. -Knowledge: healthy lifestyle. Adverse effects of tobacco use- 4- substantial. -Strategies for tobacco cessation- 2- limited knowledge. -Knowledge of reputable health care: resources- 1- no knowledge. |
Nursing Notes
Discussed readiness for enhanced self-care considering his living situation with Mr. Sampson and his friend Joe. Mr. Sampson and Butch have demonstrated proper blood sugar monitoring techniques and insulin administration using hospital equipment over the last two days. He has witnessed and participated in dressing changes to the left toe as well.
Mr. Sampson has his first appointment for IV antibiotic administration and dressing change at the ambulatory care clinic tomorrow at 0900, and both he and Joe acknowledge their knowledge of the location and how they will get there. Outpatient PT has been arranged with the PT department .
Mr. Sampson has had instruction and practice keeping his PICC line dressing clean. He leaves here today with a clean, labeled dressing on his left toe and PICC line, and the following prescriptions:
Metformin 1000mg PO BID
Lantus 10 units SQ Daily
Insulin syringes 50 count
Glucose test strips 100 count
Medical Records for his visit have been forwarded to County Healthcare.
Physical Therapy
PHYSICAL THERAPY
Initial Evaluation - Day 2 of admission
S: ”I just hate being penned up in here. I know they say it’s for my own good but I just want to get out and be on my own again. They’re telling me I can’t go back to living on the street but that’s home for me. I won’t be able to stay in a shelter again- no freedom there and too many rules. All I need is to finish these antibiotics and be able to walk again, and I can manage on my own.”
O:
History: Patient admitted yesterday for treatment of infected left foot, and poor control of type 2 diabetes. Also has history of tinnitus in both ears. Patient was independent in mobility and self care prior to his admission.
Social: Currently homeless. Receives health care through the VA clinic. He states he has no family here in Phoenix, but has a friend that has been helping him. Smokes tobacco (one pack/day).
Precautions: Must wear OrthoWedge shoe when ambulating
Standard Examination findings:
Observation: Patient lying semi-reclined in bed has IV in right forearm. Left foot wrapped in dressing/ace wrap
Cognition/language: Alert, oriented to time, place and person. Consistently follows instructions.
Sensation: Light touch and kinesthesia is decreased but not absent in both ankles and right foot. Left foot wrapped in dressing/ace wrap, and not tested. Sensation proximal to ankles intact in bilateral LEs. Denies pain in left foot, even with weight bearing.
Motor: Active range of motion WNL.
Tone: WNL.
Strength: 4/5 hip flexors and knee extensors; 4-/5 hip abductors; 4/5 ankle dorsiflexors and (R) plantarflexors.
Balance: Independent sitting. Required minimum assist from sit to stand at bedside.
Modified Clinical Test of Sensory Integration on Balance: Able to maintain standing eyes open on firm surface 30 secs without increased sway; able to maintain balance with eyes closed for 5 seconds on level surface with eyes closed. Unable to balance on foam without significant sway, eyes open or closed. Able to stand on right leg for 3 seconds eyes open; unable to stand on right leg with eyes closed. Unable to stand on left leg independently. Functional Reach Test: unable; required minimum assist to maintain balance when attempting to reach.
Mobility: Independent bed mobility. Required minimum assist from sit to stand at bedside. Modified independent transfers moving between bed and bedside chair. Patient able to walk 45 feet x2 using front wheeled walker with minimum assist to advance walker. Stairclimbing/steps not assessed. Timed 10-Meter Walk Test using front wheeled walker at a comfortable gait speed was 0.5 m/s. OrthoWedge shoe worn throughout standing and gait activities.
Wound Management: Elastic wrap and betadine-soaked gauze dressing removed. Wound bed contains 100% red viable tissue. No malodor detected. Wound edges are sloped. Periwound is pink with no evidence of streaking, induration, or maceration. Silver-impregnated packing strips moistened with sterile water applied to the wound bed. Skin protectant applied to intact surrounding skin to prevent maceration. Thin foam dressing applied as a secondary dressing and foot wrapped in gauze elastic wrap to secure.
A: Major impairments and activity limitations include:
- Lower extremity weakness.
- Limited endurance.
- Impaired single-leg stance balance; impaired ability to use vestibular information for balance, or reach outside of base of support.
- Minimum assist for transfer- sit to stand.
- Reduced gait speed.
- Minimum assist with walker for walking indoors on level surfaces.
- Open wound on weight-bearing surface.
Goals:
- Increase strength lower extremities ½ grade for increased use in activities of dialing living.
- Maintain standing on foam eyes open for 10 seconds to increase ability to use vestibular information for balance.
- Modified independence with sit to stand transfers moving between bed and bedside chair
- Modified independence walking to bathroom with assistive device.
- Ambulation with assistive device 150’ level surfaces.
Plan: Therapeutic exercise and mobility training 1-2x/day. Progress distance walked. Patient education. Discharge planning. Monitor and promote wound healing with nursing. Order needed equipment. Discharge wound dressing changes to nursing care since there is no skilled PT need at this time. PT to monitor nursing wound notes and will resume care, if skilled need is indicated.
PHYSICAL THERAPY
Discharge Summary - Day 7 of admission
S: “I feel stronger, I think I am ready to go out on my own and back to my routine. But they tell me I have to go to a home until I’m ready to be on my own.”
O: Patient has been seen 1-2x/daily during this admission. He is being discharged today to a transitional home for veterans. Patient denies pain.
Examination findings:
Cognition/language: Alert, oriented to time, place and person. Consistently follows instructions.
Sensation: Light touch and kinesthesia distal to ankles bilaterally and intact proximal to ankles
Motor: Active Range of Motion WNL.
Tone: WNL.
Strength: 4+/5 hip flexors; 4/5 knee extensors; 4-/5 hip abductors; 4+/5 ankle dorsiflexors and R plantarflexors. Strength testing of L plantarflexors deferred.
Balance:Modified Clinical Test for Sensory Interaction in Balance (CTSIB): Able to maintain standing eyes open on firm surface 30 secs and eyes closed for 20 secs without increased sway; able to maintain standing eyes open 20 secs on foam without increased sway; mild increased sway standing on foam eyes closed 10 secs. Stands on one leg eyes open right lower extremity 10 secs, left lower extremity 2 secs; eyes closed right lower extremity 3 sec and left lower extremity 1 sec. Functional reach test 15 cm.
Mobility: Modified independent transfers moving between bed and bedside chair. Modified independence for walking to bathroom with a front wheeled walker. Patient is able to walk 200 feet using a front wheeled walker at this time. Slow gait speed continues – comfortable gait speed on 10-meter walk test is 1.1 m/sec. Able to ascend and descending a 6” step with the walker and minimal assistance.
Wound Management: No skilled PT need at this time. Nursing is performing all dressing changes.
A: Patient made progress toward goals during this admission. Continues to have impairments of lower extremity weakness, limited endurance, and impaired motor and sensory strategies for balance. Has activity limitations and a need for assistive device for walking and reduced gait speed and decreased endurance requiring rest periods. Needs continued therapy to progress toward goal of independent and safe mobility. As he becomes more mobile, he will need to experience walking in longer distances and his need for assistive devices will need ongoing assessment. He needs continued balance assessment and intervention. He will need an environmental assessment prior to discharge from the transitional living facility to ensure independence and safety his prior living environment. Patient’s friend John has observed patient in therapy and feels he will be able to “watch out for him”. Patient has potential to progress to independent ambulation with ongoing rehabilitation and will need to engage in life-long fitness activities as tolerated.
Goals: Progress toward goals:
- Increase strength of lower extremities ½ grade for increased use in activities of dialing living. Partially achieved
- Maintain standing on foam eyes open for 10 seconds to increase ability to use vestibular information for balance. Achieved
- Modified independence with sit to stand transfers moving between bed and bedside chair Achieved
- Modified independence walking to bathroom with assistive device. Achieved
- Ambulation with assistive device 150’ level surfaces. Achieved
Plan: Patient to be discharged to transitional living facility. He will be followed by home health PT to maximize level of functional mobility.
Podiatry
Podiatry Notes
Operative Report
The patient was brought to the operating room and placed on the operating table in the supine position. MAC local anesthesia was provided by the anesthesia team. A calf tourniquet was placed to the lower extremity which was not inflated through the procedure. The surgical extremity was prepped and draped in the normal sterile fashion. A time out was taken and the correct patient, procedure, and extremity was verified.
Attention was directed to the affected hallux where the degenerative ulcerated tissues were removed with a #15 blade. There was underlying purulence present which was drained. There was no tunneling, tracking proximally or infected appearing tissue proximal to the hallux at this point. Infected degenerative tissue was removed from the wound and sent for microbiological examination. The ulceration unfortunately did extend to bone. After irrigated a small sample of bone was obtained with a clean rongeur. This was sent for microbiological and pathological examination. The surgical site was then washed with 3L of sterile saline in pulse lavage fashion. The ulceration was packed with betadine soaked ¼ inch nu gauze packing and a dry dressing applied.
Micro Culture and Sensitivity Report
Pathology Report
Gross: A 3mm diameter x 3mm piece of osseous tissue is obtained in a sterile specimen cup.
Micro exam: Osseous tissue is prepared and sliced. This is viewed with H and E staining. Present is a mix of cortical and cancellous osseous tissue with inflammatory cells present. There are leukocytes and monocytes noted within the cancellous tissue.
Discharge Summary
The patient was hospitalized with a diabetic foot infection. He has undergone surgical I and D along with cultures while in the hospital. He has been maintained on IV antibiotics and dressing changes have been performed. He has been bearing weight according to physical therapy recommendations. Upon discharge he will require daily dressing changes. 6-8 weeks of IV antibiotics (recommend vancomycin due to daily dosing). This will require weekly lab draws including BUN, Cr, ESR, CRP, CBC as well. Request pharmacy consult to adjust antibiotic dosing per renal function. Dressing changes and weight bearing per physical therapy.
Social Work Assessment
Patient Name: Butch Sampson
Presenting Medical Concerns: Patient is being referred to social services due to history of uncontrolled diabetes, low-income, and homelessness.
Insurance/Finances: Patient has Medicare part A and B and also receives some medical benefits through the Veteran’s Administration. He collects Social Security (retirement) which is approximately $1000.00 per month. Patient reports he applied for disability benefits through the VA a while ago but was denied.
Legal: Patient does not have a medical POA or advanced directives.
Primary Care Physician/Pharmacy: Patient receives healthcare at the Healthcare for Homeless Vets office in downtown Phoenix.
Psychosocial Information:
Type of Residence: Homeless. Lives in downtown Phoenix under the Interstate.
Patient lives with: Camps with Joe and “a couple of other guys.”
Family/Spouse/S.O. Information: Patient reports two ex-wives. States he gets a call every Christmas from one of them but could not say who.
Next of Kin: None identified
Level of Function: Patient states he is able to manage his day to day affairs, keep his bills paid, show up to appointments etc.
Supplies at Home: Patient states he limits the amount of “stuff” he carries.
Community Services: Patient reports he sees a social worker, John, at the Healthcare for Homeless Veterans office.
Psychosocial Stressors:
Alcohol/Substance Use/Tobacco Use: Patient states he drinks very infrequently, but smokes about one pack of cigarettes a day.
Psychiatric History: History of Depression with panic attacks. Off and on since discharge from the military.
Adjustment to Illness: Loss of toes and difficulty with walking making it more difficult to live on the streets.
Recent Lifestyle/Residence Changes: Has been on the streets for years.
Family Dynamics: No ongoing contact with family. Reports his friend Joe as his family.
Spiritual and Cultural Assessment: Not assessed.
Assessment and Anticipated Discharge Needs: S/O- Patient reports long history of homelessness but states he “gets by.” States he uses his Social Security to buy food, pay for his cell phone, bus fare, cigarettes and occasionally goes to the laundromat to wash his clothes. He notes that he has his check auto deposited into his Chase Bank Account and that the people at the bank are “real nice” to him. Patient states that he is not bothered much by the loss of his toes but reports that it is difficult for him to get around. He reports that he goes to the Healthcare for Homeless Vets office for a majority of his needs. States he sees a social worker named John that helps him. The patient noted that he tried to live in transitional housing but that he “did not like all the rules.” In relationship to family, he reports being married twice. “Didn’t work out” he states. Patient states that he gets a telephone call from one of his ex-wives every Christmas but could not remember which one. The patient adds that he has a friend named Joe that he sticks with but does not always trust the other guys on the street. Patient states he wants to get out of the hospital as soon as possible and return to the streets.
A-Patient has a clear plan for his discharge that is not consistent with his needs. He appears to be struggling with managing his life more specifically his health care needs. He does not seem to follow a proper diabetic diet nor does he seem to take medications as prescribed. In turn, this exacerbates his diabetes. For this reason, patient should be discharged to a SNF or rehab facility, then assessed for long-term needs. Patient also has some basic needs for clothing such as socks and boots. Patient’s support system is very limited and patient would benefit from expanding his support network.
P-Discharge to SNF or rehab facility. Address needs for stable housing, nutrition counseling, access to healthcare, and reapplying to VA for disability benefits.
Completed by: Leah Mosely, LCSW
Notes From Last Dental Assessment
Dental Notes
S:
A 73 y/o Caucasian male presents for a comprehensive exam
CC:
“Sore in my mouth but. I have no teeth for the dentist to see me”.
MED HX:
Illnesses: T2DM x 5years
Injuries: Injured his back lifting cement bags in 1985
Hospitalizations: Toe amputation possibly 2015
Surgeries: Amputation Lt 4 th and 5 th Toe, unsure of date, possibly 2015
Medications:
Metformin 1000 mg PO BID
Insulin Lantus 10 Units SQ QD x 1 month
Benadryl 25-50 mg at HS prn insomnia
APAP 1000mg prn
Allergies: NKDA
Pt denies Cardiovascular, Pulmonary, Renal, Hepatic, Osteoporosis, Joint Replacement, GI, & Cancer Conditions
ALLERGIES: NKDA
DENT HX:
-Pt has been wearing U/L denture for the past approx. 30-35 years.
Ill-fitting denture, but no complain.
Sore tongue
Pt doesn’t understand why he is being visited by the dentist since he has no teeth in his mouth!
SOCIAL HX:
Occupation: retired heavy construction worker, served in armed services, Navy
Marital Status: Divorced x 2
Support: Homeless,
ETOH: “couple of beers” occassionally
Tobacco: Smokes 1pack a day
Illicit drugs: denies
Family History: No children. Support from fellow homeless veterans.
EXAM CHARTING
O:
VITALS: BP: 114/64 HR: 64 Resp:14 (Welch Allyn)
HARD TISSUE FINDINGS:
All teeth missing
Clinical Exam:
EOE: raised, firm nodule on L temporal region near hairline 10mmx6mm, L forehead 1/2 inch x 1/2 inch
Rubbery- hard R submandibular lymphadenopathy with pain
IOE:
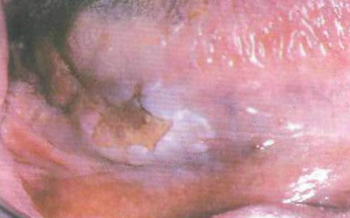
Redness around the corner of the mouth.
Red and white and mixed irregular patchy lesion with central ulceration with indurated border on the R lateral border of the tongue.
CMS/FMX, Panoramic
Maxillary Sinuses: NSF
Temporomandibular joints/condyles: Short condylar neck
Other findings: NSF
CAMBRA – N/A
Evaluated by:
STOP-BANG
OBSTRUCTIVE SLEEP APNEA SCREENING
- S-noring: Yes
- T-iredness/Fatigue: No
- O-bserved apnea: No
- P-ressure: No
- B-ody mass index: No
- A-ge: Yes
- N-eck size: No
- G-ender: No
A:
Candidiasis / Angular cheilitis
Perio Dx: N/A
Caries risk: N/A
OSA – Hi risk
Information About Other Professions
Athletic Training
Professional Domains
Athletic Trainers are educated to provide comprehensive patient care in five domains of clinical practice.
- Injury and Wellness Prevention
- Examination, Assessment, and Diagnosis
- Immediate and emergency care
- Therapeutic Intervention
- Healthcare Administration and Professional Responsibility
Clinical Learning
Athletic Trainers pass competencies in clinical learning to prepare them to possess the skills and clinical abilities along with a broad scope of foundational behaviors of professional practice.
- Evidence-based practice
- Prevention and health promotion
- Clinical examination and diagnosis
- Acute care of injury and illness
- Therapeutic interventions
- Psychosocial strategies and referral
- Health care administration
- Professional development and responsibility
CCCC Athletic Training Notes
Mr. Sampson
Can refer/find information regarding hospice care
Recognize mental health issues and understand referral strategies
Provide wound care for the foot
Gait analysis and exercises to help with gait
Proper use of cane
Walking exercises
Monitoring for infection and adverse effects
Diabetes education and insulin checks
Provide simple exercises to maintain cardiovascular and muscle tone
Provide simple exercises to maintain cardiovascular and muscle tone (in home exercises that can use what is already available)
Encourage to attend follow up appointments – suggest methods to travel if appropriate
Suggesting community support groups
Pharmacological education – proper use of medication and storage
Health Education
Health Education Consult - Hospital Notes and Assessment
Seven Areas of Responsibility: Certified Health Education Specialist
Area I: Assess Needs, Resources and Capacity for Health Education/Promotion
Area II: Plan Health Education/Promotion
Area III: Implement Health Education/Promotion
Area IV: Conduct Evaluation and Research Related to Health Education/Promotion
Area V: Administer and Manage Health Education/Promotion
Area VI: Serve as a Health Education/Promotion Resource Person
Area VII. Communicate, Promote, and Advocate for Health, Health Education/Promotion, and the Profession
Certified Health Education Specialist (CHES) “Consult” - Health Education/Community and Public Health:
HEALTH EDUCATION SPECIALIST – TRANSITION/DISCHARGE NOTES AND RESOURCES
The Health Education Specialist may be found in the Military/Navy Public Health Center and would work with the healthcare team to Prevent Disease, Promote Health, and Keep Communities Safe https://www.med.navy.mil/sites/nmcphc/Pages/Home.aspx
https://www.health.mil/Military-Health-Topics/Operation-Live-Well
“Health Educators plan and implement evidence-based programs/interventions, so I would recommend some resources/programs/education for Butch….”
DIABETES:
VA RESOURCES/BENEFITS
https://www.benefits.va.gov/compensation/claims-postservice-agent_orange-diabetes.asp
https://www.nutrition.va.gov/diabetes.asp
https://www.nutrition.va.gov/Get_Help_From_A_Dietitian.asp
https://www.thediabetescouncil.com/useful-resource-links-for-veterans/
https://www.veteranshealthlibrary.org/LivingWith/Diabetes/
https://www.benefits.va.gov/benefits/Applying.asp
http://hbexplorer.vacloud.us/
https://www.va.gov/directory/guide/division.asp?dnum=1&isFlash=0; https://www.vets.gov/facilities/?facilityType=vet_center
PATIENT EDUCATION RESOURCES/DIABETES SELF-MANAGEMENT
https://professional.diabetes.org/search/site/diabetes%2520self%2520managment?f%5B0%5D=im_field_dbp_ct%3A32&retain-filters=1
http://care.diabetesjournals.org/content/diacare/early/2017/07/26/dci17-0025.full.pdf
https://professional.diabetes.org/content/diabetes-educator-resources
http://www.diabetes.org/diabetes-basics/?loc=db-slabnav
http://www.diabetes.org/about-us/contact-us/center-for-information.html?loc=lwd-slabnav
https://www.cdc.gov/diabetes/home/index.html
DIABETES MANAGEMENT/ADHERENCE RESOURCES
https://professional.diabetes.org/search/site?f%5B0%5D=im_field_dbp_ct%3A32&retain-filters=1
http://www.ada-ksw.com/order_diabetesPro.html
https://www.cdc.gov/diabetes/ndep/people-with-diabetes/index.html
DIABETES/DIET RESOURCES
https://professional.diabetes.org/content-page/what-can-i-eat
http://www.diabetes.org/diabetes-basics/?loc=db-slabnav
DIABETES/PUBLIC HEALTH AND COMMUNITY RESOURCES
https://professional.diabetes.org/erp_list_zip
http://www.diabetes.org/in-my-community/local-offices/phoenix-arizona/
https://www.diabeteseducator.org/living-with-diabetes/find-an-education-program
https://www.cdc.gov/diabetes/programs/national-dpp-maps/index.html
TOBACCO USE/CESSATION:
VA RESOURCES/BENEFITS
https://www.mentalhealth.va.gov/quit-tobacco/index.asp; https://www.mentalhealth.va.gov/quit-tobacco/how-to-quit.asp
https://smokefree.gov/tools-tips/text-programs/quit-for-good/smokefreevet?utm_source=facebook&utm_medium=social&utm_campaign=vet
http://hbexplorer.vacloud.us/
https://www.va.gov/directory/guide/division.asp?dnum=1&isFlash=0; https://www.vets.gov/facilities/?facilityType=vet_center
https://www.med.navy.mil/sites/nmcphc/health-promotion/tobacco-free-living/Pages/Tobacco-ForYouSelfHelp.aspx
https://tricare.mil/ucanquit2
https://health.mil/Military-Health-Topics/Operation-Live-Well/Focus-Areas/TobaccoFree-Living
SMOKING CESSATION EDUCATION RESOURCES
http://www.lung.org/stop-smoking/smoking-facts/
http://www.lung.org/stop-smoking/i-want-to-quit/
https://www.mentalhealth.va.gov/quit-tobacco/learn-more.asp
https://www.cdc.gov/tobacco/campaign/tips/groups/military.html
SMOKING CESSATION PUBLIC HEALTH AND COMMUNITY RESOURCES
http://www.lung.org/our-initiatives/education-and-training/take-a-class.html
http://www.lung.org/our-initiatives/education-and-training/get-health-education-materials.html
http://www.lung.org/support-and-community/
HOUSING
VA RESOURCES/BENEFITS
https://benefits.va.gov/BENEFITS/factsheets/limitedincome/Homeless.pdf
https://www.va.gov/homeless/for_homeless_veterans.asp
https://www.va.gov/homeless/for_at_risk_veterans.asp
https://www.va.gov/homeless/index.asp
https://www.va.gov/homeless/housing.asp
Health Education: Community/Public Health
Profession Description :
The U.S. Department of Labor Bureau of Labor Statistics (BLS) defines health educators (SOC 21-1091.00) as those who promote, maintain, and improve individual and community health by assisting individuals and communities to adopt healthy behaviors, collect and analyze data to identify community needs prior to planning, implementing, monitoring, and evaluating programs designed to encourage healthy lifestyles, policies and environments. They may also serve as a resource to assist individuals, other professionals, or the community, and may administer fiscal resources for health education https://www.bls.gov/oes/current/oes211091.htm
Health educators work to encourage healthy lifestyles and wellness through educating individuals and communities about behaviors that promote healthy living and prevent diseases and other health problems.
Responsibilities and Competencies for Health Education Specialists:http://www.nchec.org/credentialing/responsibilities/
Seven Areas of Responsibility:
Area I: Assess Needs, Resources and Capacity for Health Education/Promotion
Area II: Plan Health Education/Promotion
Area III: Implement Health Education/Promotion
Area IV: Conduct Evaluation and Research Related to Health Education/Promotion
Area V: Administer and Manage Health Education/Promotion
Area VI: Serve as a Health Education/Promotion Resource Person
Area VII. Communicate, Promote, and Advocate for Health, Health Education/Promotion, and the Profession
Brief: Certified Health Education Specialists/Roles and Responsibilities:http://www.sophe.org/healthedspecialist.cfm
Brief Videos: What is Public Health/This is Public Health/Public Health Return on Investment:
https://www.youtube.com/watch?v=ErBECLCWNOk
https://www.youtube.com/watch?v=oy1CAMObRzc
https://www.youtube.com/watch?v=B5M9JefYxJI

